Designing Optimal Diagnostic Pathways with AI
Balancing Sensitivity and Specificity for Patient Safety
This article discusses the concepts of sensitivity and specificity in AI-assisted radiology and their role in determining diagnostic accuracy. The optimal balance between sensitivity and specificity depends on the clinical context, and radiologists play a crucial role in setting the appropriate operating point for the AI algorithm. Radiologists should review all AI reports and use their clinical judgment to determine when the AI output can be relied upon.
Today we're going to talk about something significant in the fields of AI and radiology - sensitivity and specificity! These two key concepts play a huge role in determining the diagnostic accuracy of AI-assisted imaging. By the end of this blog, you'll have a solid understanding of what sensitivity and specificity are, how they can be applied in AI-assisted radiology, and why radiologists must understand these concepts.
Understanding Sensitivity and Specificity
Let's start with the basics. Sensitivity and specificity are measures of how well a test or diagnostic tool can correctly identify a condition. Sensitivity refers to the proportion of positive cases correctly identified by the test. In other words, it's the test's ability to correctly identify people who have the condition. Specificity, on the other hand, refers to the proportion of negative cases that are correctly identified by the test. It's the test's ability to correctly identify people who don't have the condition.
Here's an example to help illustrate this. Let's say we're testing for a certain type of cancer. A test with high sensitivity would correctly identify most people with the cancer. It would have a high true positive rate and a low rate of false negatives. A test with high specificity would instead correctly identify most people without the cancer. It would have a high true negative rate or a low rate of false positives.
It's important to note that a test with high sensitivity may have lower specificity and vice versa. For example, a test that has a high sensitivity for detecting a certain type of cancer may also have a high rate of false positives (i.e., it may identify some people as having the cancer who actually don't). On the other hand, a test with high specificity may have a lower sensitivity (i.e., it may miss some cases of the cancer).
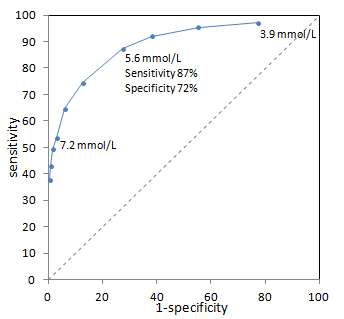
Now, let's talk about something called an operating point. This specific point on the receiver operating characteristic (ROC) curve represents the balance between sensitivity and specificity for a particular test or diagnostic tool. The ROC curve is a graphical representation of the trade-off between sensitivity and specificity, and the operating point is the point on the curve that represents the desired balance of these two factors. The operating point can be adjusted to optimize the diagnostic performance of the test or tool based on the specific clinical scenario and the characteristics of the population.
Not all Findings are Made Equal
So, why is this critical in the clinical setting? Well, the optimal balance between sensitivity and specificity depends on the clinical context, such as the type of patient and the stage of the disease. For example, in a screening population, it's important to have high sensitivity to catch as many cases as possible, even if it leads to a higher rate of false positives. In contrast, in a diagnostic population, it's vital to have high specificity to rule out a serious condition and look for other causes of the patient's symptoms.
It's also worth noting that AI usually outputs multiple findings per modality. Certain findings may require a higher sensitivity while others may require a higher specificity. For example, in a chest x-ray, it's important to have a high sensitivity for detecting small lung nodules, as these can be early indicators of lung cancer. On the other hand, pleural effusions may require high specificity, as a false positive result could lead to unnecessary invasive procedures.

Consider a 60-year-old man who comes in with a persistent cough and shortness of breath. We run an AI-assisted imaging system on the chest x-ray and it detects a small lung nodule. In this case, the AI needs to be able to detect small lung nodules because early detection of lung cancer can greatly improve the patient's outcome. If the AI had missed the nodule, the cancer could have progressed to a more advanced stage before it was detected.
Now, let's talk about a 75-year-old woman who comes in with chest pain and difficulty breathing. We get a chest x-ray and the AI detects a pleural effusion. In this scenario, the AI must have high specificity for detecting pleural effusions. If the AI incorrectly identified a pleural effusion, the patient may have undergone an invasive procedure for a condition they didn't have. This would cause unnecessary discomfort and risk.
The Radiologist's Role in Navigating AI-Assisted Diagnosis
It's pretty amazing how AI has the potential to greatly improve diagnostic accuracy. But, radiologists need to understand the limitations of the technology and how to use it in a clinically relevant manner. One key aspect is setting the appropriate operating point for the AI algorithm, which involves balancing sensitivity and specificity based on the specific clinical scenario. Radiologists play a crucial role in this process, as they have the medical expertise to determine the appropriate operating point for each case and ensure that the AI is being used in a clinically appropriate manner.

Another important thing for radiologists to keep in mind is that they should review all AI reports and use their clinical judgement to decide when the AI output can be relied upon and when a human review is required. This can help radiologists focus on more complex cases that need their attention and expertise, while still being able to see more patients overall. It's not unlike other technological tools like PACS, which have also helped radiologists see more patients and streamline their workflow.
AI can greatly enhance the role of radiologists as diagnostic extenders by streamlining the diagnostic process for referring physicians. Radiologists can use AI to improve the accuracy of diagnoses by ensuring that the right information is shared with the right people at the right time. They can also identify and implement appropriate AI software, monitor and maintain these tools for quality and safety, and offer AI-based diagnostic support as a service to referring physicians. By embracing AI in their practice, radiologists can take the lead in this transformation and strengthen their position as a valuable resource for healthcare enterprises.
Conclusion
In summary, AI has the potential to revolutionize the way radiologists diagnose and treat patients. By embracing AI and utilizing it in their practice, radiologists can streamline the diagnostic process for everyone in the hospital. However, radiologists must understand the key concepts of sensitivity and specificity, as well as how to balance them based on the specific clinical scenario. Radiologists also play a vital role in setting the appropriate operating point for the AI algorithm and reviewing AI reports to ensure human review is required when necessary. By gaining a deeper understanding of these concepts and utilizing AI in a clinically appropriate manner, radiologists can be key partners in integrating AI into the medical field and helping improve the quality of care for patients.